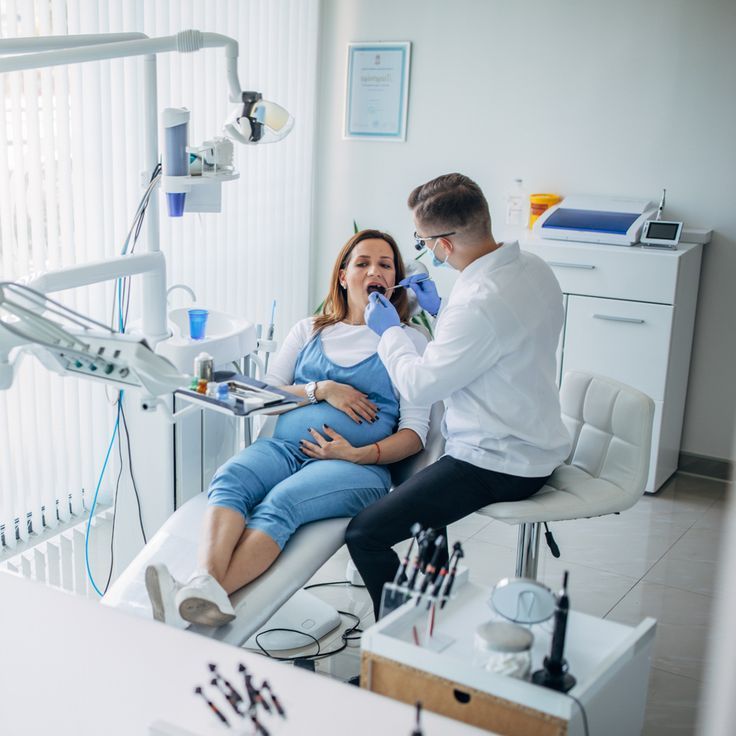
Pregnancy is a time of rapid change for every part of the body — and the mouth is no exception. Hormonal shifts, dietary changes, morning sickness, and the demands of growing a baby all affect oral health in ways that surprise many first-time mothers. The good news is that with thoughtful planning and a few simple adjustments, you can protect your smile throughout the entire journey. Here is a trimester-by-trimester dental guide for expecting mothers.
Why Pregnancy Affects Oral Health
Pregnancy raises levels of estrogen and progesterone, which change the way gum tissue responds to the bacteria that live in plaque. The result is that even normal levels of plaque can trigger more inflammation than they normally would — a condition called pregnancy gingivitis that affects most pregnant women to some degree. Additional factors compound the risk:
Morning sickness exposes teeth to stomach acid. Cravings (and snacking) can mean more frequent acid attacks on enamel. Calcium and vitamin demand increases dramatically. Dry mouth from breathing changes can develop. And dental visits sometimes get postponed because mothers worry about safety, when actually skipping care creates more risk than addressing problems.
The First Trimester (Weeks 1-12)
Common issues: Morning sickness, food aversions, dry mouth, the start of pregnancy gingivitis.
What to do:
Tell your dentist you are pregnant or trying to conceive. Many routine procedures can be done safely during pregnancy, but your dentist will adjust timing, positioning, and medications accordingly. Schedule a check-up early in pregnancy if you have not had one recently — addressing small problems now prevents emergencies later.
Do not brush immediately after vomiting. Stomach acid temporarily softens enamel. Rinse your mouth with water (a teaspoon of baking soda in water is even better) and wait 30 minutes before brushing. Brushing too soon literally wears the softened enamel away.
If toothpaste smells trigger nausea, try a milder children-flavored toothpaste, or just brush gently with water until taste tolerance returns. Skipping brushing entirely creates much bigger problems quickly.
Stay hydrated, especially if morning sickness is heavy. Dehydration concentrates whatever stomach acid does reach your mouth.
Avoid X-rays in the first trimester unless they are urgent. Most clinics will defer non-essential X-rays until the second trimester.
The Second Trimester (Weeks 13-27)
Common issues: Pregnancy gingivitis becomes more pronounced. Some women develop a benign growth on the gums called a “pregnancy tumor” (despite the scary name, it is harmless).
What to do:
This is the safest and most comfortable window for most dental treatment. If you need fillings, deep cleanings, or other routine work, the second trimester is the ideal time to schedule it. The baby is past the most sensitive stage of development, and you are usually past the worst of morning sickness.
Schedule a professional cleaning. A thorough plaque and tartar removal helps prevent gingivitis from progressing, and your dentist can give you targeted advice for any inflammation already present.
Floss every single day, without fail. Pregnancy gingivitis is largely driven by plaque between the teeth, where toothbrushes cannot reach. If your gums bleed when you floss, that means they need flossing more — not less.
Keep meals balanced and protein-rich. Calcium-rich foods (yogurt, cheese, leafy greens, fortified plant milks) support both your developing baby and your own oral health. Avoid the temptation to snack constantly on sugary or starchy foods.
If a pregnancy tumor appears on the gums, do not panic. They are not actually tumors — they are a benign overgrowth of inflamed tissue that often shrinks on its own after delivery. Your dentist can monitor it and remove it if it bothers you.
The Third Trimester (Weeks 28-40)
Common issues: Comfort during long appointments becomes harder. Back pain, heartburn, frequent bathroom needs, and pressure on the inferior vena cava when lying flat all complicate dental visits.
What to do:
Schedule shorter appointments and avoid lying flat on your back for too long. Most clinics will adjust the chair to a comfortable tilted position. If you start feeling dizzy or short of breath, shift onto your left side and let your dental team know.
Major elective procedures are usually postponed until after delivery. Focus on essential care: addressing pain, infection, or untreated decay. Cosmetic procedures and elective whitening should wait.
Maintain your home routine. Many third-trimester mothers experience heartburn or acid reflux that brings stomach acid into the mouth. Rinse with water after reflux episodes and wait 30 minutes before brushing.
Discuss postpartum dental care with your dentist. Plan to come in within the first few months after delivery for a thorough check-up and cleaning.
What About X-Rays?
Modern dental X-rays use very low doses of radiation, and the lead apron covers the abdomen for additional protection. Routine X-rays are typically postponed during pregnancy out of caution, but emergency X-rays for pain, infection, or trauma are considered safe with proper shielding. The risk of an untreated infection is almost always higher than the risk of a single X-ray.
What About Local Anesthesia and Medications?
Local anesthetics like lidocaine are considered safe at typical dental doses. Your dentist will choose formulations without epinephrine when appropriate. Most antibiotics commonly used in dentistry (amoxicillin, clindamycin, penicillin) are safe during pregnancy. Tetracycline and similar antibiotics are avoided because they can stain the developing baby’s teeth.
For pain control after a procedure, acetaminophen is generally considered safe. NSAIDs like ibuprofen are typically avoided, especially in the third trimester. Always confirm with both your dentist and your obstetrician.
Common Pregnancy Dental Myths
“The baby takes calcium from my teeth.” Not true. Calcium for the baby comes from your bones and diet, not your teeth. The cavity risk during pregnancy is from diet and hygiene changes, not calcium loss.
“I should skip the dentist while pregnant.” The opposite is true. Routine and necessary dental care is safe and recommended throughout pregnancy.
“Bleeding gums are normal during pregnancy and will go away.” Mild inflammation is common, but bleeding gums are still a sign of gingivitis that should be treated. Untreated, it can progress to periodontitis, which is associated with preterm birth in some studies.
After Baby Arrives
The first six months postpartum are a great time to catch up on any deferred dental work and have a thorough cleaning. Caring for an infant often means letting your own routine slide — make a point of brushing and flossing even on the most exhausting days. Your future smile, and the example you set for your child, both depend on it.
The Takeaway
Pregnancy isn’t a time to put your dental care on hold — it’s a time to be more thoughtful about it. With a knowledgeable dentist, a steady home routine, and trimester-appropriate timing, you can move through pregnancy with a healthy, comfortable smile and clear peace of mind. If you are pregnant or planning to be, book a check-up. The earlier you start, the smoother the next nine months will be.