If you snore loudly, wake up gasping at night, feel exhausted after a full night of sleep, or have been told you stop breathing while sleeping, you may be one of the millions of people living with sleep apnea — often without a diagnosis. What surprises many patients is that the right place to start the conversation is often the dentist’s office. Dentists are increasingly trained to spot signs of sleep apnea and to offer one of the most effective non-CPAP treatments available: custom oral appliances.
What Is Sleep Apnea?
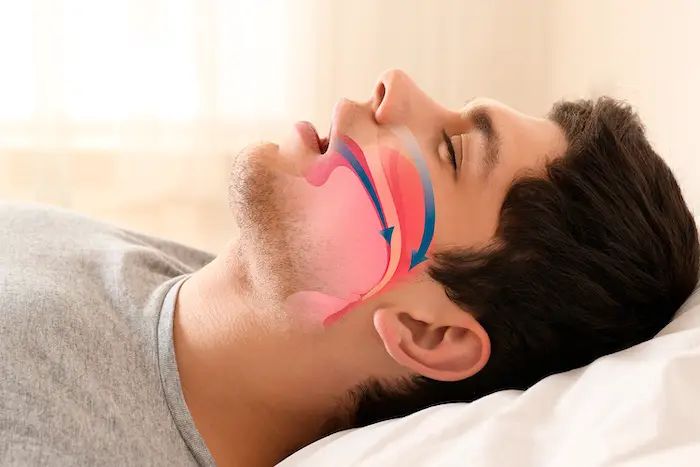
Sleep apnea is a disorder in which breathing repeatedly stops and starts during sleep. The most common form, obstructive sleep apnea (OSA), happens when the muscles in the throat relax too much during sleep and partially or completely block the airway. Each pause in breathing can last 10 seconds to a minute or more, and the brain briefly wakes the body to restart breathing — often dozens or hundreds of times per night.
The result is fragmented sleep, dropped oxygen levels, and a cascade of daytime and long-term health consequences. Untreated sleep apnea is associated with high blood pressure, heart disease, stroke, type 2 diabetes, weight gain, depression, and a higher risk of accidents.
How Dentists Recognize Sleep Apnea
Dentists see inside the mouth more often than physicians do, and several patterns suggest a higher likelihood of OSA:
Worn or flattened tooth surfaces from nighttime grinding (which often accompanies apnea). Scalloped edges on the sides of the tongue (from pressing against the teeth at night). A narrow, high-arched palate. Enlarged tonsils or a small lower jaw that crowds the airway. Tongue tie or unusual tongue positioning. Visible enlargement of the soft palate or uvula. Dry mouth and morning headaches mentioned by the patient.
A dentist who notices these signs can refer the patient for a proper sleep study — the gold standard for diagnosing sleep apnea — and then collaborate on treatment based on the diagnosis.
The Diagnostic Process
If sleep apnea is suspected, the next step is a sleep study (polysomnography). This can be done in two ways:
In-lab study: An overnight test at a sleep center where breathing, oxygen levels, heart rate, brain waves, and muscle activity are recorded in detail.
Home sleep test: A simpler version using a portable device that records breathing patterns and oxygen levels at home. Good for screening straightforward cases.
The results categorize sleep apnea as mild, moderate, or severe based on the number of breathing events per hour (apnea-hypopnea index, AHI). A diagnosis of sleep apnea opens up several treatment paths.
The Treatment Options
CPAP (Continuous Positive Airway Pressure): A mask connected to a machine that gently blows air into the airway to keep it open during sleep. CPAP is the most effective single treatment for moderate and severe OSA. The challenge is that many patients find masks uncomfortable, claustrophobic, or hard to travel with, and adherence rates are far from perfect.
Oral appliance therapy (OAT): A custom-fitted device that looks like a sports mouthguard. Worn during sleep, it gently moves the lower jaw forward, which keeps the airway open. Oral appliances are most effective for mild to moderate sleep apnea and for patients who cannot tolerate CPAP.
Lifestyle changes: Weight loss, side sleeping, avoiding alcohol before bed, and treating nasal congestion all reduce sleep apnea severity. For mild cases, these may be enough.
Surgery: Various surgical procedures can remove or reshape airway-blocking tissue, advance the jaw, or in severe cases, restructure the upper and lower jaws. Surgery is usually reserved for patients who haven’t responded to other treatments.
Why Dentist-Made Oral Appliances Work
The dental approach to sleep apnea — known as dental sleep medicine — has grown significantly over the last decade. Custom oral appliances are quiet, portable, and well-tolerated by most patients. They are typically used:
For mild to moderate OSA as a first-line treatment. For severe OSA when the patient cannot tolerate CPAP. As a backup for CPAP users during travel. In combination with CPAP at lower pressure settings.
A properly designed appliance is made from impressions or digital scans of your teeth, and it gradually advances the lower jaw to the position that keeps the airway open without straining the jaw joint. Adjustments are made over several follow-up visits until the optimal setting is reached.
What to Expect from an Oral Appliance
The fitting process usually takes two appointments over a few weeks. After delivery, you wear the appliance every night during sleep. Most patients adapt within a week or two. Some experience minor side effects:
Jaw soreness in the morning (usually resolves within weeks). Tooth tenderness. Mild changes in bite that often settle when the appliance is removed during the day. Extra saliva or temporary dry mouth.
Long-term, some patients experience small changes in tooth position. Your dentist will monitor your bite during follow-up visits and adjust accordingly.
How to Tell If You Should Be Evaluated
If two or more of the following sound familiar, ask your dentist or physician about a sleep evaluation:
Loud, chronic snoring that disrupts your bed partner. Witnessed pauses in breathing or gasping during sleep. Waking up with a dry mouth or sore throat. Morning headaches. Excessive daytime sleepiness even after a full night of sleep. Difficulty concentrating, memory problems, or mood changes. Falling asleep during the day, especially while driving. High blood pressure that is hard to control.
Who Is at Higher Risk?
Sleep apnea is more common in men, in adults over 40, in people with neck circumference greater than 17 inches (men) or 16 inches (women), in those with a family history of sleep apnea, in patients with high blood pressure or type 2 diabetes, and in people who are overweight. But it can affect thin, fit, healthy people too — body type is just one factor.
The Connection to Overall Health
Treating sleep apnea isn’t just about feeling less tired (though that is a major benefit). The long-term consequences of untreated sleep apnea make this a serious health issue. Studies link it to a roughly two- to four-fold increase in cardiovascular events, a higher stroke risk, worse blood sugar control in diabetics, and significantly higher all-cause mortality. Treatment dramatically improves outcomes.
You may also notice changes that aren’t on the official medical list: more energy, better mood, improved memory, better sex life, and a happier bed partner.
Working with the Right Team
If sleep apnea is on your radar, the right care involves both medical and dental expertise. A sleep physician confirms the diagnosis and provides the medical oversight. A dentist trained in dental sleep medicine fits the appliance and monitors your dental health during treatment. The two work together for the best outcome.
The Takeaway
Sleep apnea is common, dangerous, and very treatable. Many of its earliest signs are visible inside the mouth, which makes the dentist’s chair an unexpectedly important place to start the conversation. If you snore loudly, wake up tired, or recognize yourself in this article, raise it at your next dental visit. A short conversation could lead to a sleep study, a custom appliance, and a transformed quality of life. The body you wake up in tomorrow morning depends on the breaths you take tonight.